| News / Science News |
Neuromelanin-sensitive MRI identified as a potential biomarker for psychosis
Researchers have shown that a type of magnetic resonance imaging — called neuromelanin-sensitive MRI (NM-MRI) — is a potential biomarker for psychosis. NM-MRI signal was found to be a marker of dopamine function in people with schizophrenia and an indicator of the severity of psychotic symptoms in people with this mental illness.
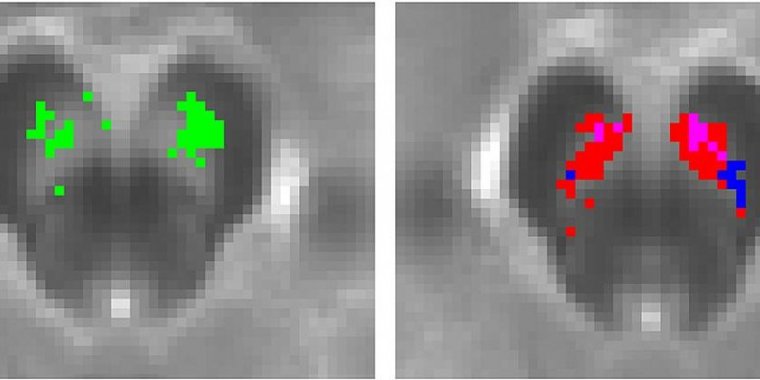
Left displays a map of substantia nigra voxels where NM-MRI signal positively correlated with PET measures of dopamine release capacity [green]. Right displays a map of substantia nigra voxels where NM-MRI signal was positively correlated with severity of psychotic symptoms; individuals with schizophrenia [red]; clinical high risk individuals [blue]; the overlap between both groups [pink]. Photo: Dr. Guillermo Horga
Disturbances affecting the neurotransmitter dopamine are associated with a host of mental and neurological disorders, such as schizophrenia and Parkinson’s disease. Because of the role dopamine plays in these disorders, the ability to measure dopamine activity is critical for furthering our understanding of these disorders, including how to best diagnose and treat them.
Neuromelanin is a dark pigment created within dopamine neurons of the midbrain — particularly in the substantia nigra, a brain area that plays a role in reward and movement.
Neuromelanin accumulates over the lifespan and is only cleared away from cells following cell death, as occurs in neurodegenerative disorders such as Parkinson’s disease.
Researchers have found that NM-MRI signal is lower in the substantia nigra of people with Parkinson’s disease, reflecting the cell death that occurs in these patients.
In this study, Guillermo Horga, M.D., Ph.D. of Columbia University, New York, and colleagues conducted a series of validation studies to show that NM-MRI can serve as a marker of dopamine function in individuals without neurodegenerative disorders.
To examine the detection ability of NM-MRI, the researchers compared NM-MRI measurements of neuromelanin to chemical measurements of neuromelanin in post-mortem brain tissue. The researchers found, across all sections of tissue, that higher NM-MRI signal was associated with higher concentrations of neuromelanin.
The results confirm, for the first time, the ability of NM-MRI to measure regional concentrations of neuromelanin. Furthermore, the results show that NM-MRI signal reflects concentrations of neuromelanin in tissue, rather than just the number of neuromelanin-containing neurons.
The researchers found decreases in NM-MRI signal in those with Parkinson’s disease in the lateral, posterior, and ventral areas of the substantia nigra — findings that correspond to the known anatomical distribution of cell loss in this brain area in Parkinson’s disease. These results confirm that NM-MRI can capture known topographical variability within this brain structure.
Individuals with a higher NM-MRI signal had greater dopamine release capacity in the striatum (a core component of reward, motor, and cognitive systems). The researchers also found that NM-MRI signal in the substantia nigra was associated with functional MRI measures of regional cerebral blood flow.
More severe symptoms of psychosis were associated with higher NM-MRI signals in the nigrostriatal pathway of individuals with schizophrenia and in those at-risk for schizophrenia. Psychosis is associated with dopamine system dysfunction, characterized by greater dopamine release and synthesis capacity in the striatum.
The findings suggest that NM-MRI is capturing this dopamine dysfunction, supporting the role of NM-MRI as a potential biomarker for psychosis. (National Institutes of Health)
YOU MAY ALSO LIKE



